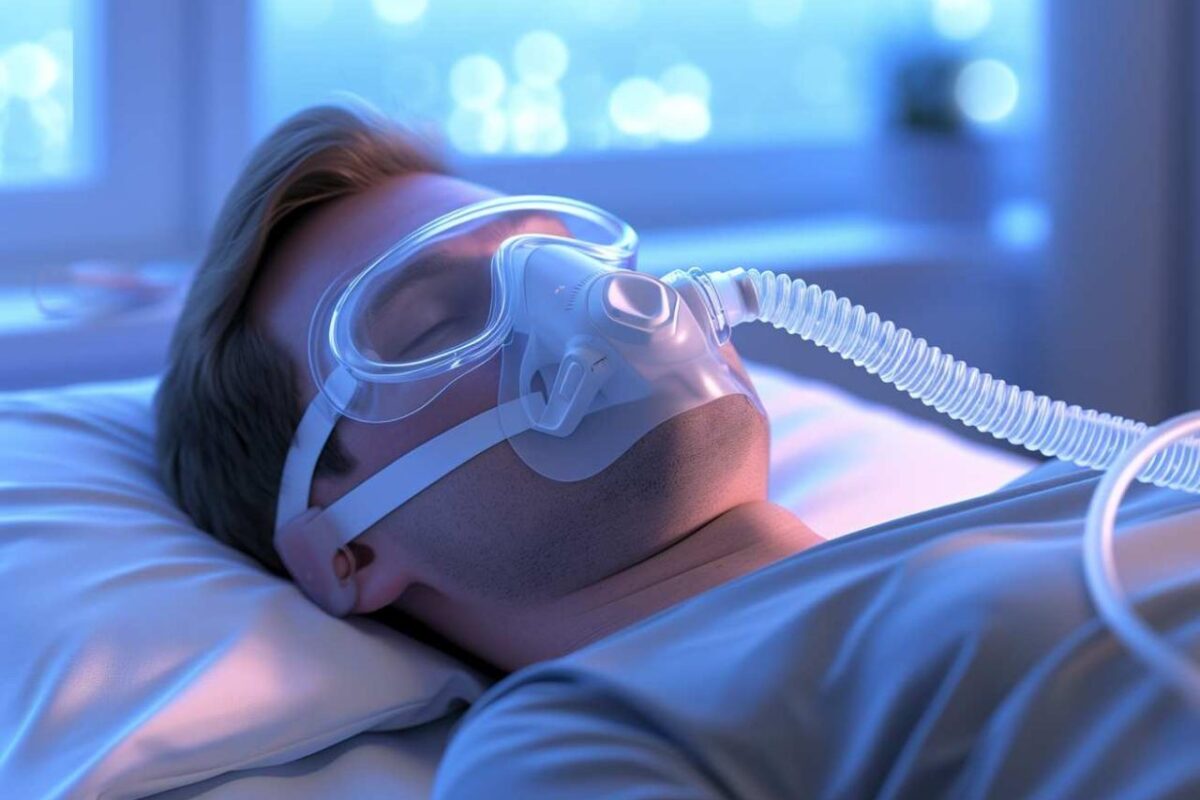
Sleep apnea is a sleep disorder that disrupts breathing during sleep, affecting millions worldwide. Characterized by pauses in breathing or shallow breaths, it can lead to a plethora of health issues if left untreated. Understanding the nuances of sleep apnea, including its types and physiological mechanisms, is crucial for recognizing its impact on daily life. From obstructive to central sleep apnea, each type presents unique challenges that require attention and intervention.
The prevalence of sleep apnea spans various demographics, making it essential to identify symptoms and risk factors. Individuals affected often experience fatigue and cognitive issues, underlining the importance of awareness and diagnosis. As we delve deeper into the intricacies of sleep apnea, we will explore diagnosis methods, treatment options, and lifestyle changes that can significantly alleviate symptoms.
Understanding the Basics of Sleep Apnea
Sleep apnea is a serious sleep disorder characterized by repeated interruptions in breathing during sleep. These interruptions can last from a few seconds to minutes and may occur multiple times throughout the night, leading to disrupted sleep patterns and a host of health concerns. The primary types of sleep apnea include obstructive sleep apnea (OSA), central sleep apnea (CSA), and complex sleep apnea syndrome, which combines elements of both OSA and CSA. OSA is the most common form, occurring when the throat muscles intermittently relax and block the airway during sleep. CSA, on the other hand, is less common and occurs when the brain fails to send the appropriate signals to the muscles that control breathing.
The physiological mechanisms leading to sleep apnea events are primarily associated with the anatomy of the upper airway and the regulation of the respiratory system. In obstructive sleep apnea, the soft tissues of the throat collapse and obstruct the airway, which leads to a decrease in oxygen levels in the blood. This triggers the brain to wake the person momentarily to reopen the airway. In central sleep apnea, the mechanism involves a failure of the brain to signal the muscles to breathe, often linked to underlying medical conditions such as heart failure or stroke. Other factors contributing to sleep apnea include obesity, age, and anatomical variations in the respiratory system.
Statistics indicate that sleep apnea affects a significant portion of the population. According to the American Academy of Sleep Medicine, it is estimated that around 22 million Americans suffer from sleep apnea, with the majority being undiagnosed. The condition is more prevalent in men than in women, with a ratio of about 2:1. It is especially common in middle-aged adults, with prevalence rates increasing with age. Additionally, sleep apnea is strongly associated with obesity, with studies suggesting that approximately 70% of individuals with OSA are overweight. Understanding these basics can help raise awareness about the condition and the importance of seeking medical advice for proper diagnosis and treatment.
Identifying Symptoms and Risk Factors of Sleep Apnea
Sleep apnea is a serious sleep disorder that often goes undiagnosed. Understanding its symptoms and the associated risk factors is crucial for early identification and management. Many individuals may overlook the signs or attribute them to other issues, making awareness essential for those at risk.
Common symptoms experienced by individuals with sleep apnea include loud snoring, which is often reported by bed partners. People may also experience frequent awakenings during the night, gasping or choking sensations, and excessive daytime sleepiness. Other symptoms can manifest as difficulty concentrating, mood changes, headaches, and a dry mouth upon waking. These symptoms can significantly disrupt daily life and overall well-being.
Symptoms and Severity Levels
Recognizing the severity of symptoms can help in assessing the potential impact of sleep apnea on an individual’s health. Below is a table that categorizes common symptoms along with their severity levels:
| Symptom | Severity Level |
|---|---|
| Loud Snoring | Moderate to Severe |
| Gasping or Choking During Sleep | Severe |
| Excessive Daytime Sleepiness | Moderate to Severe |
| Frequent Nighttime Awakenings | Moderate |
| Difficulty Concentrating | Moderate |
| Mood Changes (Irritability, Depression) | Moderate |
| Morning Headaches | Moderate |
| Dry Mouth Upon Waking | Mild |
Several risk factors increase the likelihood of developing sleep apnea. These include obesity, which significantly raises the risk due to excess fat around the neck and throat. Age is another factor, as sleep apnea is more prevalent in older adults. Gender plays a role, with men being more likely to develop the condition than women. Other risk factors include family history, smoking, and excessive alcohol consumption, which can exacerbate throat relaxation during sleep. Certain medical conditions like high blood pressure and diabetes also contribute to the risk of sleep apnea. The combination of these factors can lead to more severe manifestations of the disorder, underlining the importance of awareness and proactive health measures.
The Diagnostic Process for Sleep Apnea

Diagnosing sleep apnea involves a comprehensive evaluation that combines medical history, physical examination, and specialized sleep studies. This multifaceted approach ensures that the condition is accurately identified and appropriate treatment options can be determined.
A crucial first step in the diagnostic process is gathering a detailed medical history. This includes discussing sleep patterns, daytime sleepiness, and any symptoms the individual may experience, such as loud snoring or gasping during sleep. Healthcare providers also inquire about lifestyle factors, such as alcohol consumption, smoking habits, and weight, which can influence the severity of sleep apnea. A physical examination typically follows, focusing on the upper airway. The physician may assess the size of the neck, the presence of any abnormalities in the throat, or other risk factors that could contribute to obstructive sleep apnea.
Role of Sleep Studies in Diagnosis
Sleep studies play a vital role in confirming the diagnosis of sleep apnea. There are primarily two types of studies: in-lab sleep studies and home sleep apnea tests.
In-lab sleep studies, also known as polysomnography, are conducted overnight in a sleep center. These tests involve monitoring various physiological parameters while the individual sleeps. The following data is typically collected during an in-lab study:
- Brain activity (EEG): Measures sleep stages and identifies disruptions.
- Eye movements (EOG): Monitors REM sleep phases.
- Muscle activity (EMG): Detects any movements that might indicate sleep disturbances.
- Heart rate and rhythm: Assesses cardiovascular health during sleep.
- Oxygen levels (pulse oximetry): Monitors oxygen saturation to detect hypoxemia.
- Airflow and breathing patterns: Observes the presence of apneas or hypopneas.
This comprehensive data allows for a precise diagnosis and the identification of the severity of sleep apnea.
Home sleep apnea tests offer a more convenient alternative for some patients. These tests can be conducted in the comfort of one’s home and typically involve a simplified setup. While they are less comprehensive than in-lab studies, they still provide essential information about breathing patterns, oxygen levels, and heart rate. Home tests are often used for patients with a high likelihood of moderate to severe obstructive sleep apnea and can provide valuable insights, though they may miss some complexities of sleep disorders.
Common Diagnostic Tools and Tests
Several diagnostic tools are utilized to confirm sleep apnea and gauge its severity. These include:
- Polysomnography: The gold standard for diagnosing sleep apnea, as previously discussed.
- Home Sleep Apnea Test (HSAT): A less intensive study performed at home, typically involving fewer monitoring channels.
- Oximetry: A simple test measuring oxygen saturation levels, often used during home tests.
- Electrocardiogram (ECG): May be performed to rule out cardiac issues related to sleep apnea.
- Sleep questionnaires: Tools like the Epworth Sleepiness Scale help assess daytime sleepiness and the likelihood of sleep apnea.
Each of these tools contributes to a comprehensive assessment of sleep apnea, allowing healthcare providers to develop effective and targeted treatment plans. Accurate diagnosis is essential because untreated sleep apnea can lead to significant health risks, including cardiovascular problems, metabolic issues, and impaired quality of life. Understanding the diagnostic process empowers individuals to seek the help they need for a healthier sleep experience.
Treatment Options Available for Sleep Apnea
Sleep apnea is a serious condition that disrupts sleep and can lead to various health issues if left untreated. Fortunately, there are multiple treatment options available that cater to different levels of severity and patient preferences. Treatments range from simple lifestyle changes to more complex medical interventions, each with its unique benefits and limitations.
Lifestyle changes often serve as the first line of defense against sleep apnea. These may include weight management, avoiding alcohol and sedatives, quitting smoking, and changing sleep positions. For some individuals, even minor adjustments can significantly improve their sleep quality. However, when lifestyle changes are insufficient, medical interventions become necessary.
Medical Treatment Options
Two primary categories of treatment options exist: non-invasive and surgical approaches. Non-invasive treatments include Continuous Positive Airway Pressure (CPAP) therapy and dental appliances, while surgical options range from minimally invasive procedures to more extensive surgeries. Each method comes with its own advantages and drawbacks, making it essential to consider which treatment aligns best with individual needs and circumstances.
CPAP therapy is widely regarded as the gold standard for treating moderate to severe sleep apnea. The device uses a steady stream of air to keep the airway open during sleep. Many patients experience immediate improvements in sleep quality; however, compliance can be challenging due to discomfort or noise from the device.
Dental appliances, such as mandibular advancement devices (MADs), reposition the jaw to keep the airway open. They can be less intrusive than CPAP machines and are often easier for patients to tolerate. However, they may be less effective for those with severe apnea and require adjustments from a dental professional.
In contrast, surgical options can provide a more permanent solution, especially in cases of anatomical blockages. Common procedures include uvulopalatopharyngoplasty (UPPP), which removes excess tissue in the throat, and maxillomandibular advancement (MMA), which repositions the jaw. While surgeries can lead to considerable improvement, they carry risks such as complications and longer recovery times.
| Treatment Method | Pros | Cons |
|---|---|---|
| CPAP Therapy |
|
|
| Dental Appliances |
|
|
| Surgical Options |
|
|
“Choosing the right treatment for sleep apnea is crucial for achieving a restful night’s sleep and improving overall health.”
Lifestyle Changes to Manage Sleep Apnea
Managing sleep apnea effectively often involves making thoughtful lifestyle changes that can significantly alleviate symptoms. Individuals suffering from this condition may find that modifying daily habits not only improves their sleep quality but also enhances their overall health. Here, we’ll explore various strategies that can lead to better management of sleep apnea, focusing on dietary changes, exercise routines, and effective sleep hygiene practices.
Dietary Changes, Exercise Routines, and Sleep Hygiene Practices
Adopting a healthy lifestyle is crucial for those dealing with sleep apnea. Implementing specific dietary changes can reduce the severity of symptoms. A diet rich in fruits, vegetables, whole grains, and lean proteins can help maintain a healthy weight and improve overall cardiovascular health. Limiting processed foods, sugars, and saturated fats is equally important, as these can contribute to weight gain and exacerbate sleep apnea symptoms.
Incorporating regular physical activity into the daily routine can also make a significant difference. Engaging in moderate exercises such as walking, cycling, or swimming for at least 150 minutes a week can help reduce body weight and improve respiratory function. Not only does exercise aid in weight management, but it also enhances sleep quality by promoting deeper, more restorative sleep.
Another vital aspect of managing sleep apnea is practicing good sleep hygiene. This includes maintaining a consistent sleep schedule, creating a restful environment, and avoiding stimulants like caffeine and nicotine before bedtime. Additionally, ensuring that sleeping positions do not obstruct airflow can be beneficial; many individuals find sleeping on their side to be helpful.
Weight management is critical, as excess weight can increase fatty deposits around the neck, leading to airway obstruction during sleep.
Maintaining a healthy weight plays a significant role in alleviating sleep apnea symptoms. Studies indicate that even a modest weight loss of 10% can lead to a substantial reduction in the severity of sleep apnea. For instance, a person weighing 200 pounds might see improvements in their condition with a weight decrease of just 20 pounds. Therefore, focusing on weight management through a balanced diet and regular exercise is essential for effective sleep apnea management.
The Impact of Sleep Apnea on Health and Daily Life
Sleep apnea, a condition characterized by repeated interruptions in breathing during sleep, can have profound effects on both physical health and day-to-day functioning. When left untreated, sleep apnea poses significant short- and long-term health risks. This discussion highlights those potential consequences, as well as how sleep apnea can alter cognitive function, mood, and overall quality of life, making it essential to address this condition seriously.
Health Consequences of Untreated Sleep Apnea
The health implications of untreated sleep apnea are extensive and alarming. In the short term, individuals may experience excessive daytime sleepiness, leading to impaired attention and diminished performance in daily tasks. This can significantly increase the risk of accidents, especially while driving or operating heavy machinery.
Long-term effects are even more concerning. Chronic sleep apnea is associated with a range of serious health issues, including cardiovascular problems such as hypertension, heart failure, and arrhythmias. Furthermore, individuals with untreated sleep apnea are at a higher risk of stroke, type 2 diabetes, and metabolic syndrome, which can contribute to further health complications.
The interplay between sleep apnea and cognitive function is significant. Many patients report difficulties with memory, decision-making, and problem-solving abilities. Studies suggest that the intermittent oxygen deprivation caused by sleep apnea may lead to changes in brain structure, particularly in areas responsible for memory and cognitive control.
In terms of mood, sleep apnea has been linked to increased levels of anxiety and depression. The chronic fatigue and disturbed sleep patterns can exacerbate feelings of irritability and frustration, leading to a diminished quality of life. Individuals often find themselves caught in a cycle of poor sleep and negative emotional states, further compounding the challenges they face.
To better understand the everyday challenges faced by those living with sleep apnea, let’s consider the following points.
Living with sleep apnea can result in multiple daily obstacles that can hinder personal and professional life. Recognizing these challenges is crucial for both patients and those around them.
- Chronic Fatigue: Persistent tiredness can make it difficult to engage fully in daily activities, affecting work productivity and personal relationships.
- Difficulty Concentrating: Impaired cognitive function can lead to challenges in tasks requiring focus, such as studying or executing complex work duties.
- Social Isolation: Individuals may avoid social situations due to embarrassment about snoring, using a CPAP machine, or not feeling well-rested.
- Health Complications: The risk of developing comorbidities may necessitate frequent medical appointments or treatments, further complicating daily life.
“Sleep apnea is more than just a sleep disorder; it’s a condition that can impact every aspect of a person’s health and well-being.”
Understanding these implications can aid in more effective management and treatment of sleep apnea, ultimately improving the quality of life for those affected.
Recent Research and Advancements in Sleep Apnea Treatments
Recent advancements in the understanding and treatment of sleep apnea have paved the way for innovative therapies that promise to improve patient outcomes significantly. Studies are increasingly focusing on personalized treatment approaches, leveraging advanced technologies and a deeper understanding of the underlying mechanisms of the disorder. This evolving landscape is not only enhancing the quality of life for individuals affected by sleep apnea but also offering new avenues for research and clinical practice.
Innovative Therapies and Technologies
Recent research has unveiled a variety of innovative treatments and technologies aimed at addressing the complexities of sleep apnea. Continuous Positive Airway Pressure (CPAP) therapy remains a cornerstone; however, new approaches are emerging. For instance, adaptive servo-ventilation (ASV) has shown promise, especially in patients with central sleep apnea. Modern devices can now respond in real-time to changes in breathing patterns, improving comfort and efficacy.
Furthermore, oral appliances designed to reposition the jaw and tongue have gained traction. A study published in the *American Journal of Respiratory and Critical Care Medicine* highlighted that customized mandibular advancement devices can reduce the severity of obstructive sleep apnea (OSA) in many patients who struggle with traditional treatments.
Phrenic nerve stimulation is another groundbreaking advancement. This treatment involves implanting a device that stimulates the phrenic nerve to promote diaphragm movement during sleep, and trials indicate significant improvements in apnea-hypopnea index (AHI) scores and overall sleep quality. This is particularly beneficial for patients who are intolerant to CPAP therapy.
The integration of telemedicine has also transformed management strategies. Remote monitoring and virtual consultations facilitate ongoing patient support and more frequent adjustments to treatment plans, leading to enhanced adherence and overall management of the condition.
These advancements in treatment modalities are associated with improved patient outcomes, including better sleep quality, decreased daytime sleepiness, and enhanced overall health. Notably, patients report increased satisfaction with their care, which is crucial in chronic conditions that require long-term management.
The future of sleep apnea research is promising, with several key directions emerging:
- Enhanced understanding of genetic and environmental factors influencing sleep apnea severity.
- Development of more effective pharmacological treatments targeting the pathophysiology of sleep apnea.
- Exploration of machine learning algorithms for diagnosing and predicting treatment outcomes.
- Investigation into combination therapies that synergize multiple treatment modalities.
- Long-term studies assessing the impact of new treatments on cardiovascular health in sleep apnea patients.
- Increased focus on the psychological aspects of living with sleep apnea and integrated care approaches.
- Advancements in home-based diagnostic tools to improve access to care.
Support Systems and Resources for Individuals with Sleep Apnea
Sleep apnea can be a challenging condition to manage, but numerous support systems and resources are available to help individuals navigate its complexities. From support groups to educational materials, these resources can make a significant difference in coping and managing the condition effectively. Having the right support can foster a sense of community, enhance understanding, and provide practical tools for those affected by sleep apnea.
Healthcare providers play a crucial role in managing and supporting patients with sleep apnea. They offer not only medical expertise but also emotional and psychological support. Patients are encouraged to establish a relationship with their healthcare providers, who can guide them through treatment options, such as Continuous Positive Airway Pressure (CPAP) therapy, lifestyle changes, or surgical interventions. Regular follow-ups are essential, as they allow healthcare providers to monitor the effectiveness of treatments and adjust them as necessary. Providers can also share valuable educational resources and connect patients with local support groups.
Available Support Systems
Various support systems are specifically designed to help individuals with sleep apnea. These can play an essential role in the journey towards managing the condition effectively.
- Support Groups: Many communities offer support groups where individuals can share their experiences, challenges, and successes related to sleep apnea. These gatherings can foster a sense of belonging and provide emotional reinforcement.
- Online Communities: Platforms like forums and social media groups allow individuals to connect with others worldwide facing similar challenges. These virtual spaces can offer 24/7 support and a wealth of shared knowledge.
- Educational Resources: Numerous organizations, such as the American Academy of Sleep Medicine, provide brochures, webinars, and online articles that educate patients about sleep apnea, its effects, and management strategies.
- Professional Counseling: Mental health professionals can help patients cope with the emotional aspects of living with sleep apnea, including anxiety and depression that may arise due to the condition’s impacts on daily life.
- Sleep Clinics: Many hospitals and health systems have specialized clinics that not only diagnose sleep apnea but also offer comprehensive care that includes education, treatment options, and ongoing support.
Personal stories and testimonials from individuals living with sleep apnea highlight the profound impact of community and support. For instance, one individual shared how joining a local support group transformed their experience; they found comfort in hearing others share similar struggles and successes. This sense of connection motivated them to stay consistent with their CPAP therapy, leading to improved sleep quality and overall well-being.
Another testimonial revealed that participation in an online forum provided a lifeline for a person feeling isolated due to their condition. Through sharing tips and receiving encouragement from others, they felt empowered to overcome challenges and better manage their sleep apnea. These personal accounts underscore the essential nature of community in navigating the complexities of sleep apnea and emphasize that no one has to face it alone.
Last Word
In conclusion, understanding sleep apnea is vital for improving both health and quality of life. With various treatment options available, including lifestyle changes and medical interventions, individuals can find effective ways to manage their symptoms. Staying informed about recent research and advancements can empower patients to take control of their health. Remember, seeking support and community resources can make a significant difference in navigating this complex condition, leading to a healthier, more restful life.
FAQ
What are the common symptoms of sleep apnea?
Common symptoms include loud snoring, choking or gasping during sleep, excessive daytime sleepiness, and difficulty concentrating.
Can sleep apnea be cured?
While sleep apnea can often be managed effectively with treatment, it may not be completely cured. Continuous management is usually required.
Is sleep apnea dangerous?
Yes, untreated sleep apnea can lead to serious health problems, including heart disease, high blood pressure, and diabetes.
Who is at risk for sleep apnea?
Risk factors include obesity, age (particularly over 40), a family history of sleep apnea, and certain anatomical features like a thick neck or enlarged tonsils.
What lifestyle changes can help with sleep apnea?
Lifestyle changes such as losing weight, avoiding alcohol, sleeping on your side, and maintaining healthy sleep hygiene can help alleviate symptoms.