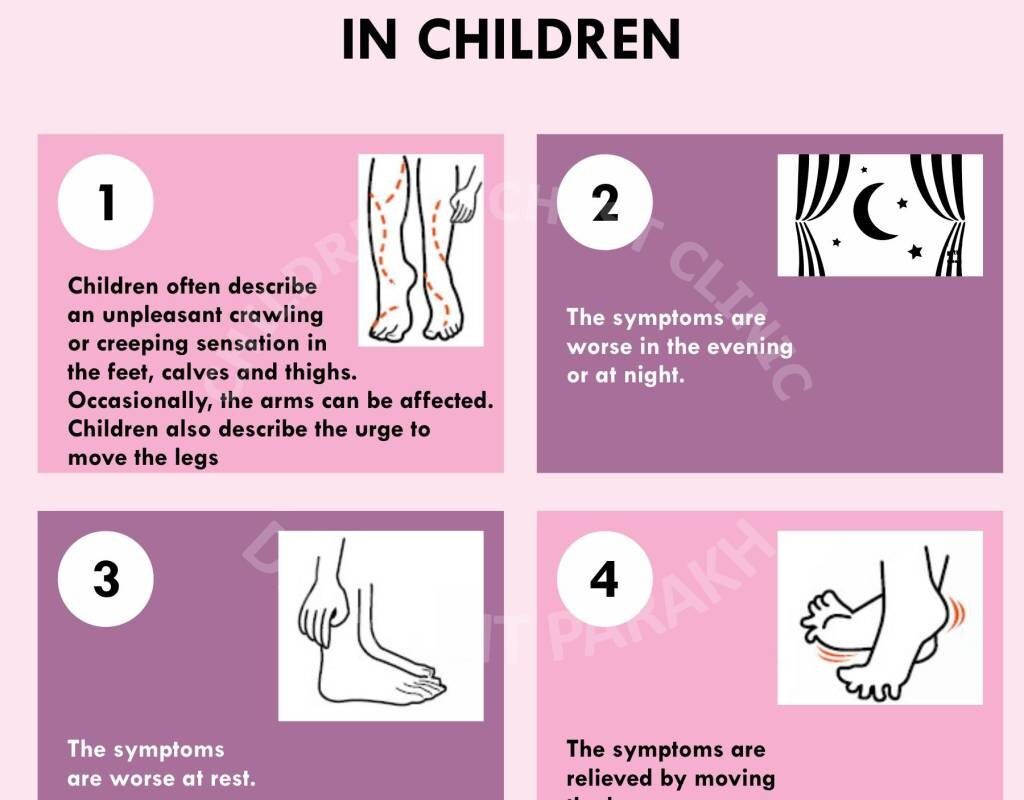
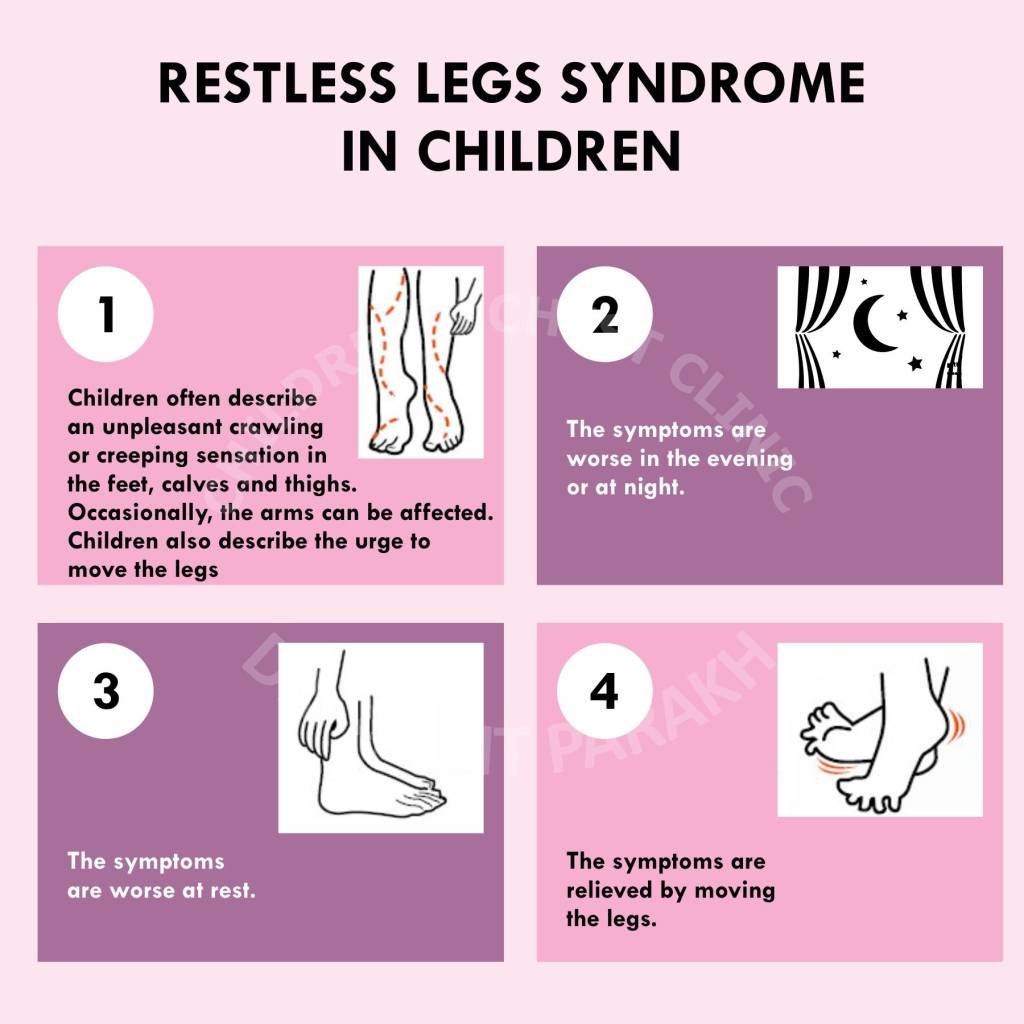
Restless leg syndrome (RLS) is more than just an occasional twitch or urge to move; it’s a neurological condition that affects millions, disrupting sleep and daily life. Often characterized by uncomfortable sensations and an irresistible urge to move the legs, RLS can lead to profound restlessness and discomfort, particularly in the evening or night. Those affected may experience symptoms that vary in intensity, making it a condition that deserves attention and understanding.
While RLS can impact anyone, it often affects specific demographic groups, including older adults and pregnant women. The exact physiological mechanisms behind RLS remain partially understood, but research suggests a link to dopamine pathways in the brain and other underlying health conditions. With growing awareness, it is crucial to delve into the diagnostic processes, treatment options, and the broader implications of living with this unique syndrome.
Restless Leg Syndrome Overview
Restless Leg Syndrome (RLS), also known as Willis-Ekbom disease, is a neurological disorder characterized by an uncontrollable and often overwhelming urge to move the legs. This condition typically manifests during periods of rest or inactivity, often leading to discomfort that can disrupt sleep and daily activities. Core symptoms include unpleasant sensations in the legs, often described as creeping, crawling, or tingling, which are temporarily relieved by movement.
The demographic groups most affected by RLS include adults, particularly those aged 40-60 years, although it can occur at any age. Women are more likely to experience RLS than men. Additionally, individuals with a family history of the condition or those suffering from chronic illnesses such as diabetes, Parkinson’s disease, or iron deficiency are at a higher risk.
Physiological Mechanisms Associated with RLS
The precise physiological mechanisms behind Restless Leg Syndrome remain somewhat elusive, but several theories have been proposed. One of the most widely accepted theories relates to dopamine dysfunction within the brain. Dopamine is a neurotransmitter that plays a critical role in controlling movement. A deficiency in dopamine, particularly in the basal ganglia, may contribute to the symptoms of RLS.
Another contributing factor could be alterations in iron metabolism. Iron is essential for dopamine synthesis, and low levels of iron in the brain have been linked to increased RLS symptoms. Studies have shown that individuals with RLS often have lower serum ferritin levels, indicating depleted iron stores.
Genetic factors are also believed to play a role, as RLS can run in families. Certain gene variations associated with iron metabolism and dopamine regulation may increase the likelihood of developing the disorder.
Current research is exploring the relationship between RLS and other conditions, including peripheral neuropathy and chronic kidney disease. Such studies aim to clarify the complex interplay between these conditions and how they may exacerbate or contribute to RLS symptoms.
Understanding the underlying mechanisms of RLS is crucial for developing effective treatment strategies.
The Diagnosis Process of Restless Leg Syndrome
Diagnosing Restless Leg Syndrome (RLS) involves a comprehensive approach that takes into consideration various criteria, medical history, and symptom tracking. Healthcare professionals rely on specific guidelines to differentiate RLS from other similar conditions, ensuring an accurate diagnosis.
The diagnosis of RLS primarily hinges on a set of established criteria. The most widely recognized criteria are based on the International Restless Legs Syndrome Study Group (IRLSSG) guidelines, which include the following:
- The urge to move the legs, accompanied by uncomfortable sensations, particularly during periods of inactivity.
- Symptoms that worsen in the evening or at night, leading to difficulty in sleep.
- Relief of symptoms with movement, such as walking or stretching.
- Symptoms that are not attributable to other medical conditions.
Understanding one’s medical history and systematically tracking symptoms play a pivotal role in the diagnosis process. Patients are often encouraged to keep a detailed record of their leg discomfort, noting the timing, frequency, and intensity of symptoms. This documentation aids healthcare providers in recognizing patterns that are characteristic of RLS. Moreover, the patient’s family history can be significant as RLS appears to have a genetic component; a family member with the condition can increase one’s likelihood of diagnosis.
Healthcare providers may also conduct various tests and examinations to rule out other conditions that could mimic RLS symptoms. These may include:
Potential Tests and Examinations
Tests are crucial for a comprehensive assessment. Here are a few examinations that may be performed:
- Blood tests to check for iron deficiency or other nutritional deficiencies.
- Polysomnography (sleep study) to observe leg movements during sleep and diagnose possible sleep disorders.
- Neurological examinations to evaluate nerve function and rule out other neurological disorders.
- Electromyography (EMG) to assess muscle activity and identify any underlying neuromuscular conditions.
In conclusion, the diagnosis of Restless Leg Syndrome is multifaceted, relying on specific criteria, comprehensive patient history, and various diagnostic tests. These elements work together to form a clear picture of the patient’s condition, ultimately leading to effective management strategies.
Common Treatment Options for Restless Leg Syndrome
Restless Leg Syndrome (RLS) can significantly impact an individual’s quality of life, prompting the need for effective management strategies. Treatment options for RLS are varied and can be tailored to each individual’s specific symptoms and health profile. They generally encompass medications, lifestyle modifications, and alternative therapies, each serving a unique role in alleviating the discomfort associated with this condition.
Medications for Managing RLS Symptoms
A range of medications are available for managing symptoms of RLS. These medications work by targeting the underlying neurological components associated with the disorder. It’s essential to consult a healthcare professional for proper evaluation and prescriptions. The main classes of medications prescribed include:
- Dopaminergic Agents: These include drugs like pramipexole and ropinirole, which increase dopamine levels in the brain, helping to relieve RLS symptoms by improving motor control.
- Gabapentin and Pregabalin: These anticonvulsants are effective in reducing symptoms of RLS by affecting neurotransmitter activity, thus helping to alleviate sensations in the legs.
- Opioids: In severe cases where other treatments are ineffective, low doses of opioids like methadone can be prescribed to help manage pain and discomfort.
- Iron Supplements: For those with low iron levels, supplements may help alleviate symptoms, as iron deficiency has been linked to RLS.
Lifestyle Changes and Home Remedies
In addition to medication, certain lifestyle changes and home remedies can significantly alleviate RLS symptoms. Adopting healthier habits may enhance overall well-being and reduce the severity of RLS. Some effective strategies include:
- Regular Exercise: Engaging in moderate physical activity, particularly during the day, can help reduce restlessness at night.
- Sleep Hygiene: Creating a sleep-conducive environment and maintaining regular sleep patterns may improve the quality of sleep and reduce RLS symptoms.
- Warm Baths and Massages: Soaking in a warm bath or receiving leg massages can promote relaxation and may temporarily ease the urge to move.
- Avoiding Stimulants: Limiting or eliminating caffeine and nicotine can significantly improve symptoms, as these substances may worsen RLS.
Conventional vs. Alternative Treatments
When managing RLS, individuals often weigh the benefits of conventional treatments against alternative therapies. Both approaches have their merits and can be effective depending on the individual’s circumstances. Conventional treatments primarily offer immediate symptom relief through medications prescribed by healthcare professionals, focusing on addressing the neurological aspects of RLS. However, they may come with side effects and dependency risks.
On the other hand, alternative treatments, such as acupuncture, yoga, and dietary supplements, focus on holistic well-being and may offer natural relief without the side effects commonly associated with pharmaceuticals. For instance, acupuncture has been shown to help some individuals by promoting relaxation and improving circulation in the legs. Additionally, incorporating essential oils, like lavender, in home relaxation practices may also provide symptom relief.
It’s crucial to consider individual preferences and health conditions when choosing between these options. A combination of both conventional and alternative methods may yield the best results, tailoring a treatment strategy that effectively addresses the unique needs of each person experiencing RLS.
The Impact of Restless Leg Syndrome on Daily Life
Restless Leg Syndrome (RLS) significantly disrupts the daily lives of those affected by this condition. Individuals with RLS often find themselves wrestling with sleep disturbances and a cascade of emotional tolls that arise from this chronic ailment. Understanding these impacts is essential for developing effective coping strategies and enhancing quality of life.
The sleep disturbances caused by RLS are profound. Many sufferers experience an overwhelming urge to move their legs, particularly at night, leading to difficulties falling asleep and maintaining restful slumber. As a result, individuals often suffer from insomnia, which further exacerbates fatigue and reduces overall health. Lack of restorative sleep can lead to a myriad of issues, including weakened immune function, increased risk of chronic illnesses, and impaired cognitive abilities.
Emotional and Psychological Implications
Living with RLS can create a challenging emotional landscape. The constant struggle against involuntary leg movements can lead to heightened levels of anxiety and depression. Feelings of isolation and frustration are common, especially as individuals may feel misunderstood by those who have not experienced the condition. The impact on social interactions can also be significant; for example, an individual might avoid gatherings or travel due to fear of symptom flare-ups, leading to further social withdrawal.
To cope with the daily challenges posed by RLS, several strategies can be effective. It is essential to establish a consistent sleep schedule, so the body learns when it is time to rest. Additionally, engaging in regular physical activity during the day can help alleviate RLS symptoms at night. Other methods include practicing relaxation techniques such as yoga or meditation and avoiding stimulants like caffeine in the evening.
“Implementing these strategies can lead to improved symptoms and a better quality of life for those living with RLS.”
Creating a supportive environment, both emotionally and physically, can also significantly impact the daily challenges faced by individuals. Seeking support from healthcare professionals and support groups can provide valuable resources and understanding.
Restless Leg Syndrome and Associated Conditions

Restless Leg Syndrome (RLS) is not just a standalone ailment; it often coexists with various health conditions, amplifying the challenges faced by those who experience it. Understanding these associated conditions is crucial for effective management and improving the quality of life for individuals with RLS.
Several health conditions are commonly linked to RLS, and recognizing these relationships can significantly impact treatment strategies. The most prevalent associated conditions include:
- Iron Deficiency: Low levels of iron in the brain can exacerbate RLS symptoms, as iron plays a vital role in dopamine production, which is crucial for regulating movement.
- Chronic Kidney Disease: Patients with kidney dysfunction often report increased RLS symptoms, possibly due to the altered metabolism of iron and other essential nutrients.
- Diabetes: Diabetic neuropathy can mimic or worsen RLS symptoms, leading to increased discomfort and disturbed sleep.
- Peripheral Neuropathy: This condition, often resulting from diabetes or other underlying health issues, can overlap with RLS symptoms, making diagnosis and treatment more complex.
- Pregnancy: Hormonal changes and increased blood volume during pregnancy can trigger RLS, particularly in the third trimester.
Significance of Addressing Comorbidities
Addressing these comorbidities is essential for a comprehensive approach to managing RLS. Treating underlying conditions such as iron deficiency or diabetes can lead to significant improvements in RLS symptoms. For instance, studies indicate that correcting iron deficiency may alleviate restless leg symptoms in approximately 60% of affected individuals, demonstrating the importance of adequate screening and treatment.
Recent research has reinforced the connection between RLS and other disorders. For example, a meta-analysis indicated that individuals with RLS are at a greater risk of developing cardiovascular diseases, highlighting the need for cardiovascular health assessments in patients diagnosed with RLS. Furthermore, the prevalence of RLS in individuals with mood disorders, such as depression and anxiety, suggests that psychological evaluation and treatment should also be part of the overall management strategy for those with RLS.
In summary, understanding the interplay between RLS and its associated conditions is vital for developing effective treatment plans. It not only aids in symptom management but also improves overall health outcomes for individuals affected by this syndrome.
Current Research Trends in Restless Leg Syndrome
Recent advancements in the understanding and treatment of Restless Leg Syndrome (RLS) have generated considerable interest within the medical community. As researchers explore the underlying mechanisms and explore innovative treatment methodologies, the future looks promising for those affected by this often debilitating condition. This progress highlights the importance of ongoing studies that could reshape therapeutic approaches and enhance the quality of life for patients living with RLS.
The significance of current research trends lies not only in the development of new treatment options but also in the investigation of the biological and environmental factors contributing to RLS. Recent studies have focused on the genetic predispositions and neurobiological pathways associated with the syndrome. Researchers are increasingly examining the role of iron metabolism, dopamine pathways, and even gut microbiota in the pathophysiology of RLS. These insights not only provide a deeper understanding of the condition but also open avenues for targeted therapies.
Emerging Treatment Modalities and Clinical Trials
The exploration of novel treatment modalities is a critical aspect of RLS research. Recent clinical trials have investigated various pharmacological therapies beyond the traditional dopaminergic agents. For example, the use of gabapentin and pregabalin, primarily known for their applications in neuropathic pain, has shown promising results in managing RLS symptoms. Additionally, opioid therapy has emerged as a viable option for severe cases, emphasizing the need for personalized treatment strategies.
Ongoing studies are also focusing on non-pharmacological interventions. For instance, behavioral therapies, mind-body techniques, and lifestyle modifications are being evaluated for their effectiveness in alleviating RLS symptoms. These approaches emphasize holistic care, recognizing the interplay between psychological and physical health in managing chronic conditions.
The role of patient participation in research is vital for advancing knowledge about RLS. Clinical trials rely heavily on the involvement of patients who can provide firsthand insights into their experiences. This participation not only enhances the data collected but also empowers patients to be active contributors to their healthcare journey. As more individuals engage in research studies, the likelihood of discovering novel treatments increases.
“Patient engagement in research can greatly enhance the understanding of Restless Leg Syndrome, paving the way for innovative therapies.”
Moreover, initiatives aiming to raise awareness about RLS and encourage participation in clinical trials are crucial. Educational campaigns can disseminate information about ongoing research opportunities and the importance of patient involvement. By fostering a collaborative environment between researchers and patients, the insights gained can lead to more effective treatments tailored to individual needs, ultimately improving outcomes for those affected by RLS.
Support Systems for Individuals with Restless Leg Syndrome
Restless Leg Syndrome (RLS) can significantly impact daily life, making it essential for individuals affected by the condition to find adequate support. Various resources, organizations, and support systems are available to assist those dealing with RLS, providing both information and community. Connecting with others facing similar challenges can make a considerable difference in managing the condition effectively.
Resources and Organizations
Numerous organizations provide valuable information and support for individuals suffering from RLS. These resources help raise awareness, promote research, and connect patients with support networks. Key organizations include the RLS Foundation, which offers educational materials, advocacy, and local support group listings. The National Sleep Foundation also provides resources related to sleep disorders, including RLS. Additionally, platforms like Reddit and Facebook have groups where members share personal experiences and coping strategies.
Role of Support Groups
Support groups play a vital role in offering emotional and practical assistance to those affected by RLS. They serve as a safe space where individuals can share their experiences, validate their feelings, and discuss coping techniques. These groups often include both in-person and online meetings, making them accessible for everyone regardless of geographic location. The shared understanding among group members fosters a sense of community, helping individuals feel less isolated.
Coping Strategies from Support Networks
Within support networks, numerous effective coping strategies are shared among members. These strategies can help mitigate the symptoms of RLS and improve overall quality of life. Here are some widely recommended techniques:
- Regular physical activity, such as walking or stretching exercises, can help relieve symptoms.
- Establishing a consistent sleep schedule encourages better rest and reduces RLS occurrences.
- A warm bath before bedtime can relax the legs and promote better sleep.
- Practicing relaxation techniques, such as meditation or deep breathing exercises, helps reduce stress.
- Applying hot or cold packs to the legs can provide temporary relief from discomfort.
- Limiting caffeine and alcohol intake can help minimize symptoms.
These strategies, suggested by individuals who understand the challenges of RLS, offer practical ways to cope with this condition. Connecting with support systems not only provides tips for managing symptoms but also fosters a community of understanding and encouragement.
Future Directions in Understanding Restless Leg Syndrome
The quest to better understand Restless Leg Syndrome (RLS) is rapidly evolving, with significant implications for both diagnosis and treatment. Research in genetics and novel therapeutic strategies is paving the way for a more comprehensive understanding of this condition, which remains enigmatic for many. As we look ahead, the exploration of genetic factors and innovative treatments is vital.
Genetic Research and Its Potential
Emerging studies suggest that genetic predisposition plays a critical role in RLS. Researchers are diving into the genetic architecture of the syndrome, aiming to identify specific genes and variants associated with RLS. This focus on genetics may not only clarify the underlying mechanisms of the disorder but also lead to the development of targeted therapies.
Recent genome-wide association studies (GWAS) have identified several loci linked to RLS, including variants in genes related to iron metabolism and dopamine signaling. This connection suggests a potential hereditary transmission of RLS, prompting further investigation into familial patterns. Identifying these genetic markers could facilitate early diagnosis and personalized treatment strategies tailored to an individual’s genetic profile.
Innovative Therapeutic Approaches
As research on RLS progresses, the development of novel therapeutic approaches is becoming more feasible. Current medication options, such as dopamine agonists and iron supplements, may be expanded upon or refined based on new findings. The exploration of gene therapy, for instance, could offer groundbreaking solutions by directly addressing the genetic mutations implicated in RLS.
Additionally, there is a growing interest in neuromodulation techniques, including transcranial magnetic stimulation (TMS) and deep brain stimulation (DBS). These methods target the brain regions associated with motor control and sensory perception, providing an alternative to traditional pharmacological treatments. Early studies have shown promising results, highlighting the need for further clinical trials to establish efficacy and safety.
Experts in the field express optimism about the future of RLS management. With advancements in technology and a deeper understanding of neurobiology, the potential for innovative treatments and improved quality of life for patients with RLS is on the horizon. The integration of genetic insights with novel therapies could lead to more effective management strategies that address the unique needs of individuals suffering from this condition.
Final Wrap-Up
In summary, understanding restless leg syndrome (RLS) is vital for both those suffering from it and their support networks. With effective diagnosis and a range of treatment options, including lifestyle adjustments and medications, individuals can manage their symptoms and improve their quality of life. As research continues to evolve, there is hope for new treatments and deeper insights into this perplexing condition, emphasizing the importance of community support and education in navigating the challenges RLS presents.
Quick FAQs
What causes restless leg syndrome (RLS)?
The exact cause of RLS is often unknown, but it can be linked to genetic factors, iron deficiency, and certain chronic conditions.
Is restless leg syndrome (RLS) hereditary?
Yes, RLS can run in families, indicating a genetic component that may contribute to its development.
Can RLS be cured?
While there is no known cure for RLS, symptoms can often be managed effectively through various treatments and lifestyle changes.
Are there specific triggers for RLS symptoms?
Certain triggers like caffeine, stress, and prolonged inactivity can exacerbate RLS symptoms for some individuals.
How is restless leg syndrome (RLS) different from periodic limb movement disorder?
RLS involves an uncontrollable urge to move the legs, often accompanied by uncomfortable sensations, while periodic limb movement disorder consists of involuntary leg movements during sleep.